Ratification Date: 02/03/2026
Next Review Date: 02/03/2027
Health Inequalities Toolkit
The majority of health and wellbeing outcomes are affected not just by access to services, but by where people live, what job they do, levels of education, socio-economic background and wider external factors as well as behavioural risks. People experiencing disadvantage in any of these areas consistently have poorer outcomes, including shorter life expectancy, worse health, and reduced quality of life.
This toolkit is designed to support multiagency partnerships to reduce these unfair and avoidable health inequalities. There are several options available for partners to scale up or down according to the need in the locality. It outlines a systematic approach across organisations and communities to identify where best to target activity to reduce inequalities and sense check prior assumptions or other data. It also supports partners to embed health equality assessments as an approach. There are four stages:
- Understand local needs
- Engage communities and agencies
- Evaluate activity and change as necessary
- Develop shared actions suitable for every party involved.
Action 1: Identify area(s) and / or population groups
You will already likely have a wide range of data available and understand your communities and areas of need. However, this is a chance to consider other data sources and sense check and challenge existing areas to see if anything has changed, been missed or not garnered sufficient attention to needs.
The working group may be interested in identifying poor outcomes for particular groups that are not consistent with other groups in localities, despite efforts of existing services in place. Take time to consider the following questions:
- What data do you already have?
- Are there gaps in the data or other factors to consider?
- If you already know which areas or populations to work in, do these decisions still stand up in the light of other data or comparisons?
Recommended links:
| What? | Details |
| A guide to using national and local data to address health inequalities. | This guide explains what is meant by inequalities data, and lists useful websites to find data for the local area. |
| Norfolk Insight | A Norfolk County Council run website with useful local and national data on a broad range of topics which can be reviewed on a place basis. It also includes detailed briefings on issues relevant to Norfolk and is a good starting point for general data. |
| JSNA and District Profiles (Norfolk Insight) | A picture of the health and wellbeing of the people of our county and the issues which affect their needs, inequalities and services. |
| Fingertips | Fingertips is run by the Department of Health and Social Care, and offers indicators across a range of health and wellbeing themes. |
| Norfolk & Waveney Digital Exclusion Heatmap | The map shows places in Norfolk and Waveney where people are less likely to have digital access opportunities. It uses local and national data to help us know where to target activity and make best use of resources. |
| Inclusion Health Dashboard | National dashboard with local data and insight on health needs and outcomes for inclusion health populations are not routinely available. The resource collates numerical population data into one place and summarises academic research and published material to highlight health needs. It is divided up into main messages, data, health overview and policy, guidance and further resources. |
| Office for National Statistics Health Index | A national set of indicators covering health outcomes, behaviours, and wider determinants. This is helpful for tracking long-term trends. |
| Office for Health Improvement and Disparities Local Authority Health Inequalities Dashboard | This tool has been developed to present evidence of health inequalities in England. Measures of inequality are provided for key indicators to monitor progress on reducing inequalities within England. |
| Wider Impacts of COVID-19 (PHE/UKHSA) | National monitoring tool that brings together metrics to assess the wider impacts of coronavirus on health.
Although no longer updated, this is still useful for contextual analysis of inequality impacts. |
| Nomis | Detailed census and labour-market data with LSOA-level breakdowns. This is helpful for socioeconomic segmentation. |
| NHS Digital datasets | This is for more technical users- especially quality/experience datasets with demographic breakdowns. |
Action 2: Identify partners and people
- What existing joint priority setting can the partnership build on?
- Which organisations will have the most influence and impact on this priority area of interest?
- Is there leadership on this priority area already or can it be encouraged through use of evidence?
- Determine governance arrangements (as minimal as possible), and appropriate levels of engagement for relevant partners and groups.
- A lead coordinating partner should be agreed, but the accountability is shared.
- Who is passionate about your chosen priority and who is missing that can add value to the process?
- How much engagement in systems approaches and integrated working is there likely to be? Realistically?
- Consider undertaking a stakeholder analysis mapping exercise. This document on Partnership Development offers a template.
Action 3: Population Intervention Triangle Assessments
This stage will help you understand what resources, activities and drivers there are within the chosen priority and locality. How much detail and time you spend on this should be determined locally. The diagram below shoes the components of the Population Intervention Triangle.
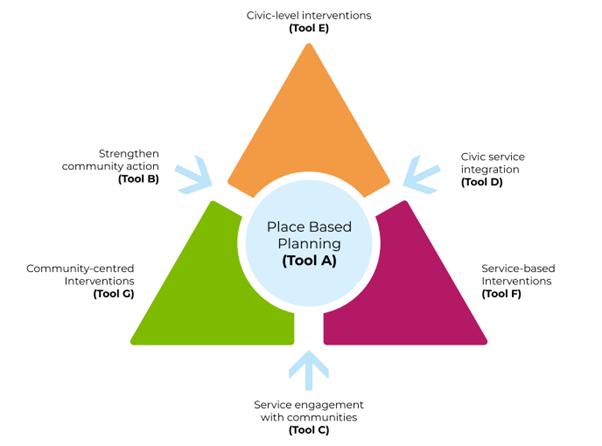
The Population Intervention Triangle maps activities by:
| What is it? | More information | Template | |
| Civic functions | It encompasses the statutory functions of the local authorities in the locality which may be locally determined or set by central government. This helps you to understand what functions the local authority already delivers to support your goals (e.g. planning, housing, community safety, economic development). | For further information on the civic level duties have a look at this section in the Population Intervention Triangle Framework for Action.
OPTIONAL: Health In All Policies
|
Civic Level Assessment template |
| Service assessments | What services already operate in the area or population. | For more information on the service assessment level have a look at this section in the Population Intervention Triangle Framework for Action.
|
Service Based Assessment template |
| Community interventions | What are the community services, functions, support networks etc. in operation. This stage is critical to understand the place and what is happening beyond the confines of statutory sector organisations and their commissioned services. In order to map current community assets, you may wish to consider the Family of Approaches Framework which maps types of community interventions such as Asset Based Community Development (ABCD). | For more information on the community interventions level, have a look at this section in the Population Intervention Triangle Framework for Action.
RECOMMENDED: Family of Approaches |
Community-centred Assessment template |
Bring it all together into an outline plan for the area/population- you can use the Locality Action Plan template with partners below to do so, or create your own plan:
| Action | Activities required | Who with? | Costs? |
Action 1: Work with communities in your area/population of choice
Having understood the community assets in your area, the next step is to consider how to ensure meaningful participation of the community and build capacity and sustainability overall. Things to consider:
- Which groups/people/representatives are members of the wider partnership already working with?
- Are any voices missing? Actively challenge this.
- Understand and review barriers to engagement.
- Be clear about what and how much can be affected by engagement process and what support may be required to deliver equality of discussion.
- Are other sectors missing which have regular impacts on people’s lives such as schools, shops, transport, informal spaces such as cafes or pubs etc.
- Are there some voices more dominant or influential and is that correct?
Core principles for engagement are:
- Consider equity, control and voice principles throughout discussions.
- Use evidence-based approaches to community engagement.
- Be clear about which decisions people in communities can influence and how this will happen.
- Respect the rights of communities to get engaged as much or as little as they are able to.
- Identify barriers to involved, particularly for vulnerable groups and recently established communities.
Action 2: Consider a community action plan
It may be useful to identify actions to build on community capacity and engagement from the community. The aim now is to develop sustained participation and engagement in the activities identified in the local development action plan. Consider what resources, champions, or agreed tasks might be and include them in the local development action plan. Consider the following:
- What needs to happen to deliver the plan made at Stage 1 and fill gaps?
- What plans are already in place across organisations which can be given a health focus?
- What assets have been identified to draw upon or expand to deliver this plan?
- How is the plan to be agreed and delivered?
- It is unlikely every agency and organisation will agree or prioritise the same things- focus on working in areas where there is agreement and ability to effect change.
Local Development Action Plan:
| Action | Activities required | Who with? | Costs? |
By this stage you will understand community capacity within your area and found ways in which to engage with communities and work with them to develop activities to reduce health inequalities and increase their capacity as appropriate.
Action 1: Consider what to evaluate and how
It may be unnecessary if the plan is to scale up an existing function that already has monitoring systems in place. Or if the working group agrees to use a tried and tested method of their own. It is for the working group to decide this, as long as partners are confident on how they can tell if they are getting the results they planned for with clear input and direction from the target population, group, or area.
Some prompts for what could be monitored and evaluated are also listed below:
Monitoring for outcomes:
Partners may wish to stop thinking solely ‘is it effective?’ and start thinking ‘does it contribute?’ to build a picture which reflects the reality. In the case of long-term change such as life expectancy, determine what evidence can be used to monitor short term interventions to impact the long-term issue. A theory of change logic model contributes to identifying what resources are needed and when by, to achieve an outcome. It will also allow the working group to begin to measure the less tangible outcomes, unintended consequences and broader impact of an action. This can be strengthened by undertaking an equality or health equity assessment exercise, which seeks out potential variations in outcomes for groups and helps planning to mitigate against them.
Monitoring value for money:
Monitoring value for money and return on investment is also advised. The success of an activity can be hindered if financially unsustainable. Consider how prevention activities can be monitored against the cost of no further action and reducing future costs. Consider the cost of activities now, and the cost of prevention activities, and monitor anticipated savings, this should contribute towards the aim of sustainability of funding in the future.
Monitoring for efficacy:
Be prepared to re-evaluate actions in the light of evidence and feedback. Monitoring what doesn’t work helps identify future actions or immediate modifications to services.
Action 2: Some further considerations
As outcomes are likely to take many years to be seen in a population, what evidence is available to decide which activities will affect those changes and can the delivery of these be assessed?
Make sure what you intend to do will directly impact what outcome you seek. It is important to capture and measure the broad benefits of what it is you intend to do, in a way that doesn’t miss some of the ‘soft’ outcomes.
Make sure what you intend to do does not adversely impact vulnerable groups, and that any mitigating action is identified if causes for concern are highlighted. We recommend undertaking a Health Equity Assessment.
OPTIONAL: A comprehensive video explaining what theory of change is as well as a practical example: Logic Models and Theory of Change
Templates for use:
RECOMMENDED: Health Equity Assessment Tool The Health Equity Assessment Tool (HEAT) should be undertaken BEFORE any intervention or planned activity is implemented, as it outlines intentions, and allows the opportunity to review potential consequences. Other tools or local processes may be in place/ The important factor is to understand impacts on both reducing health inequalities and considering unintended consequences to the contrary.
OPTIONAL: Theory of Change, Logic Model Template
OPTIONAL: RE-AIM tool The RE-AIM tool outlines a simple way to measure the success of the activities outlined in the local development plan against five key measures. Reach, Effectiveness, Adoption, Implementation, Maintenance.
OPTIONAL: Ripple Effects Mapping is a participatory, qualitative method that can capture the wider (intended and unintended) impacts of a project or programme. It brings together people who have been involved in, or affected by, the delivery of a project or programme to visually map out what they have done and the impacts to date.
By this stage you will have a clear idea of what you want to do, and when you will assess progress (proportionate to what you do and resource), and what success may look like.
By this stage, there should be clarity on what organisations, partners, communities, and stakeholders can affect. For example, access to good quality long term employment is unlikely to be in the sole gift of one local organisation as wider economic and social factors will be at play. However, your organisations may be able to work to improve access to education or decide as a group to directly employ local labour or support mental health tin workplaces to contribute to the outcome sought.
This is also an opportunity to review what should stay the same in order to avoid worsening of outcomes. Not everything will work so be prepared to make changes. Equally some things may take a while to have an effect or be taken up by the target area or group.
Practical considerations for implications:
- Has the group identified what resources are required? This could be staff, physical assets like buildings, or funding for example.
- Has the group identified how to communicate planned actions to the wider stakeholder groups?
- Is the community on board and part of the solution?
- Outline what workforce changes may need to take place such as training or integrating service delivery.
- Ensure that capacity to change has been built into the planned activity so that what is not working can be monitored and adapted.
- Has the working group been given the go ahead by the agreed governance structure?
RECOMMENDED: Local Area Development Plan template (in Stage 2, Action 2).
OPTIONAL: Theory of Change- logic modelling
OPTIONAL: NICE guidance principles
This toolkit has been designed to aid partners in planning for equitable health outcomes for residents. Partners will have considered the issues from a broad range of perspectives, with community assets and voices at the centre of discussions. The range of tools in the toolkit will have aided the partnership to distil the information down to core actions. The local area development action plan begun in the first staged can be updated to reflect what partners know, what they intend to do, who will do it and when by.
The health inequalities toolkit has been collated using a range of published tools, to help and guide Norfolk place-based organisations to tackle health inequalities. In time they will be accompanied by additional resources, including case studies, lessons learned and tailored tools.
The toolkit does not replace existing knowledge and experience of communities, residents, and organisations in the locality and should be utilised to enhance rather than dictate what is taking place in the local area. It should be viewed as a menu of options that inform a comprehensive framework, flexible enough to use sparingly or in full.

